Chronic pain care that finally makes sense.
A mechanism‑based clinical reasoning layer that matches patients to the right treatments earlier. Improving resource efficiency, strengthening clinical decisions, and elevating outcomes across high‑cost chronic pain populations.
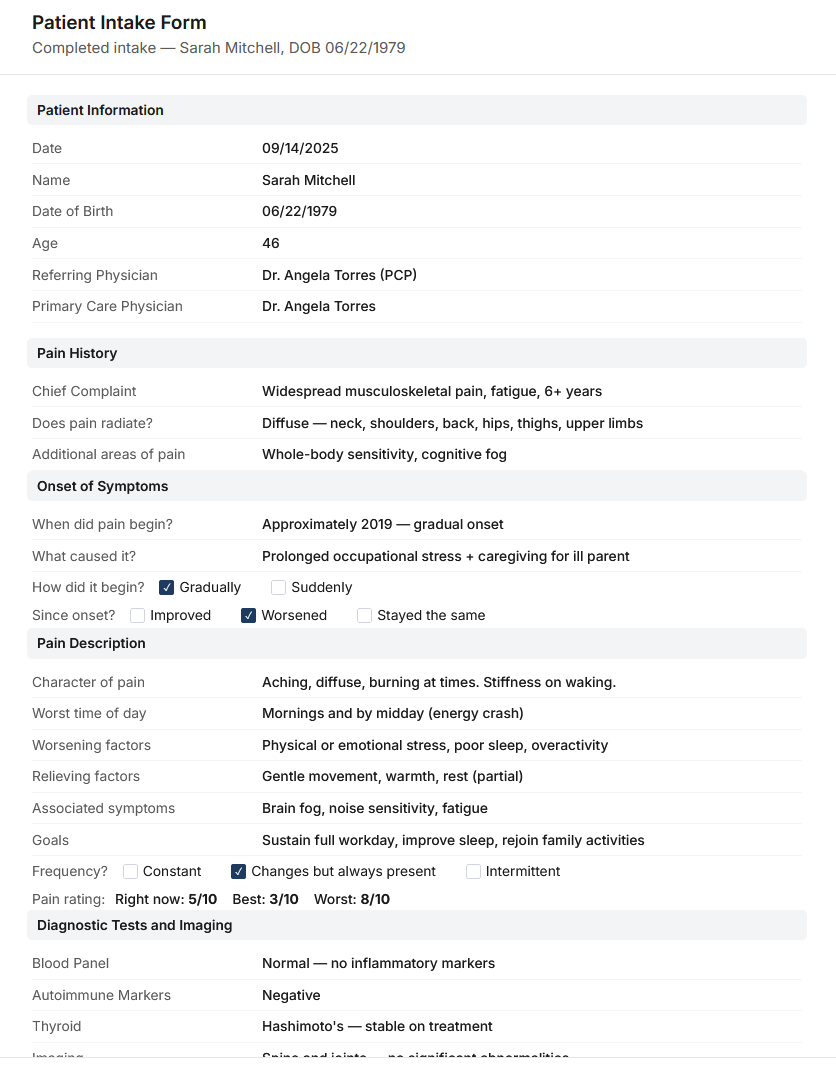

Chronic pain care is fragmented, reactive, and expensive.
Patients cycle through tests, medications, and specialists without clear answers — while clinicians face cognitive overload and payers absorb rising costs.
Fragmented Care
Patients bounce between providers without coordination. Each provider sees a fragment — no one sees the full picture.
Overuse of Imaging and procedures
MRIs and procedures are ordered outside of clinical guidelines. High cost, low diagnostic and therapeutic yield.
Polypharmacy
Medications stack up. Side effects compound. The original problem gets buried under layers of pharmaceutical management.
Clinician Burnout
Cognitive overload from clinical complexity. Pressure to act without clear direction. Morale erodes.
Poor Outcomes
Pain persists, function declines. Patients lose trust. The system labels them as 'difficult' or 'malingering'.
Reduced Access
Insurers tighten controls. Coverage gaps widen. The cycle perpetuates itself — more fragmentation, more cost, less care.
EtioLinksAI presents
PainMAP
The first product built on our clinical reasoning engine.
A clinical decision layer embedded in existing care workflows.
Chronic pain care, redesigned for primary care.
PainMAP is a mechanism-based, workflow-integrated reasoning layer that identifies what's keeping pain chronic and matches patients to evidence-aligned pathways.
Assess
Structured intake + mechanism signals
Patient data flows in — history, symptoms, treatments, imaging, medications. PainMAP identifies the signals that reveal what's maintaining the condition.
Classify
Biological, behavioral, and contextual drivers
The engine classifies pain mechanisms, drivers and dynamics across multiple dimensions — not just where it hurts, but why it persists and the underlying conditions.
Match
Evidence-aligned pathways tailored to the individual
Each patient gets a matched care pathway based on their specific mechanism profile — not a generic guideline, but a personalized pathway.
Assess
Structured intake + mechanism signals
Patient data flows in — history, symptoms, treatments, imaging, medications. PainMAP identifies the signals that reveal what's maintaining the condition.
Classify
Biological, behavioral, and contextual drivers
The engine classifies pain mechanisms, drivers and dynamics across multiple dimensions — not just where it hurts, but why it persists and the underlying conditions.
Match
Evidence-aligned pathways tailored to the individual
Each patient gets a matched care pathway based on their specific mechanism profile — not a generic guideline, but a personalized pathway.
How PainMAP works.
Three steps that integrate into how you practice.
Fits into existing consultations, coordination, and follow-up.
01
Intake
Structured from existing records or a quick form.
02
Reasoning
Mechanism classification, mismatch detection, safety screening.
03
Decision
Targeted care direction, risk flags, and a confidence score.
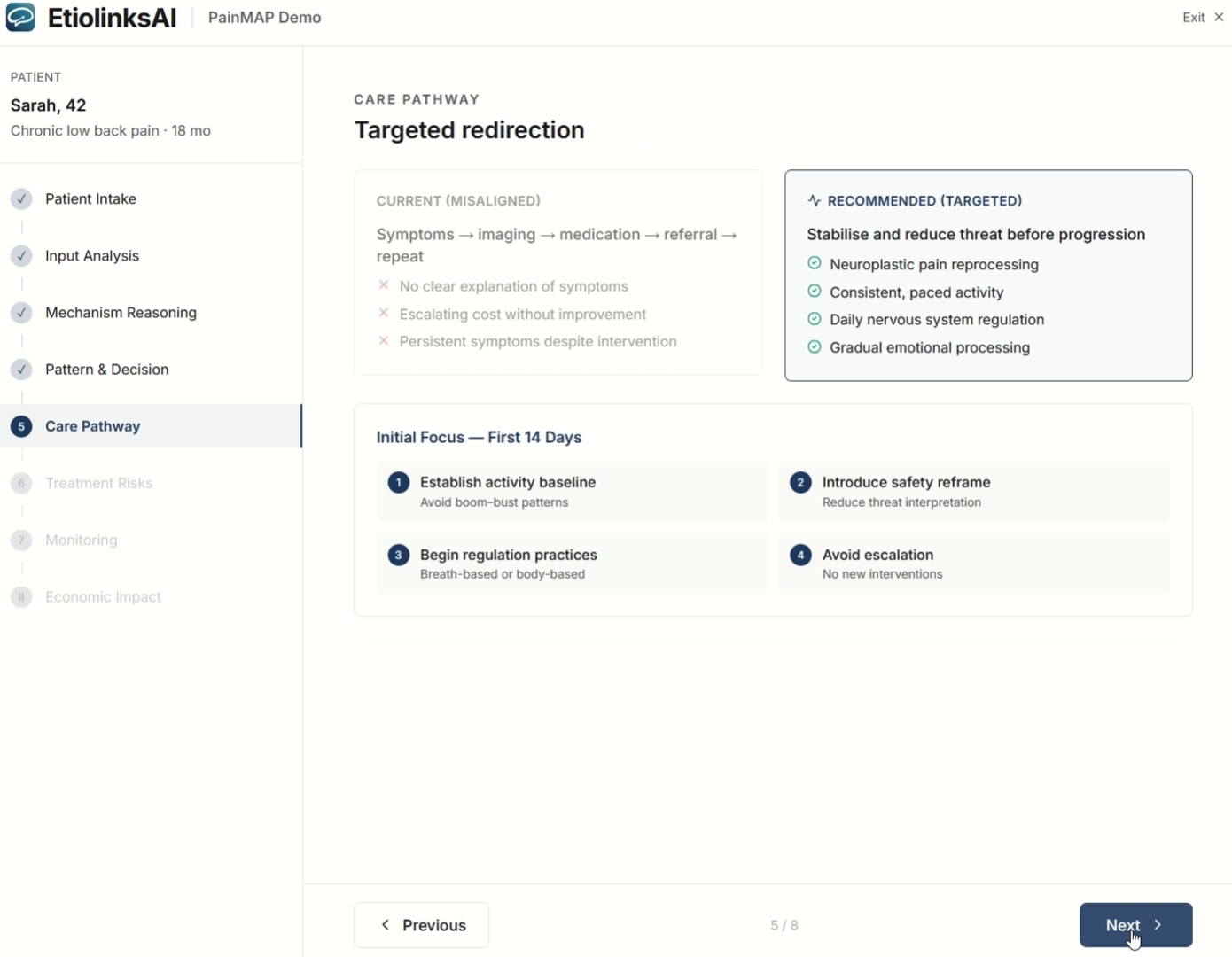
What changes with EtioLinks.
Improves decision clarity and reduces misdirected care.
PainMAP answers the question health systems currently cannot: which care pathway gives patients the best probability of meaningful outcome, and which interventions are contraindicated or premature.
We stopped ordering MRIs for every chronic back pain patient. PainMAP identified that most were central sensitization — imaging wasn't going to change the plan.
— Primary Care Physician


See it in action
See PainMAP in action.
Watch a complete assessment of a complex case. Mechanism classification, care direction, and risk flags, with full reasoning visible at every step.
- Patient completes intake prior to seeing clinician.
- Reports generated in minutes.
Grounded in evidence.
Frequently Asked Questions
What is EtioLinksAI?
A clinical reasoning platform focused on mechanism-based chronic pain care in primary care settings.
How does PainMAP work?
It structures intake, classifies mechanisms, and matches patients to evidence-aligned pathways with full reasoning visible.
Does this replace clinician judgment?
No. It augments clinical reasoning and preserves clinician autonomy, with transparent, auditable logic.
What conditions does it cover?
PainMAP currently covers chronic pain. The EtioLinksAI engine is expanding to IBS, pelvic pain, migraine, fatigue syndromes, and other conditions where symptoms and findings do not align.
Who pays for this?
Typically health systems and payers, through value-based care, care management, or innovation budgets.
How does PainMAP fit into existing billing and workflows?
PainMAP supports decision-making, care planning, and coordination already occurring within consultations and chronic care management. It does not require a new billing model.